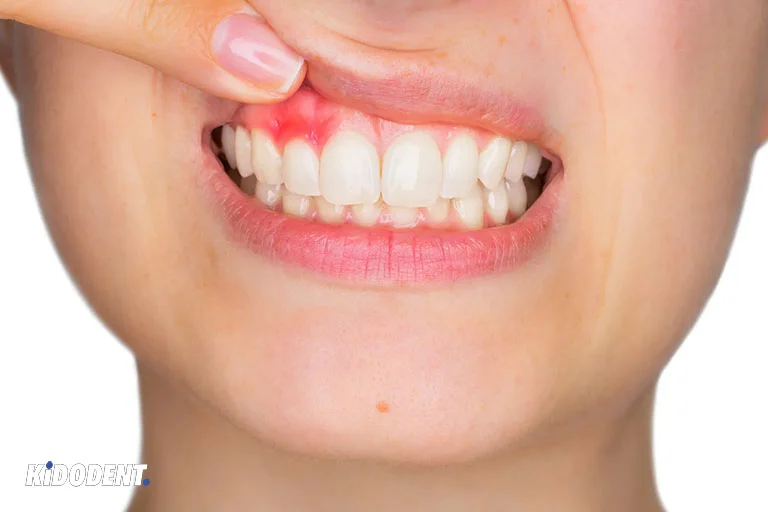
What is a dental abscess?
A dental abscess, or tooth abscess, is a pocket of pus caused by bacterial infection. It is a localized lesion that is formed into a collection of pus in or around the tooth as a result of an infection. Dental abscess occurs due to cavities or decay, injuries to tooth, gum diseases or even having a previous dental operation. The untreated infection (pus) builds up and results in tooth abscess that can spread to both soft and bone tissues near the abscessed tooth.
Tooth abscess occurs in different regions of the infected teeth and inside the gum. You can find the abscessed tooth in two main forms:
- Periapical abscess.
It occurs at the apex or tip of the tooth’s root. The bacterial infection enters the dental pulp through chips and cracks which are caused by injuries or longtime cavities and tooth decay. Dental pulp is the inner soft tissues with dental nerves, blood vessels, and connective tissues. As the pulp is infected, the infection can spread down to the root parts and form a dental abscess.
- Periodontal abscess.
A periodontal abscess occurs in the gum tissue at the side of the area surrounding teeth. The infection begins as gingivitis, which is the early stage of gum disease, and then progresses to periodontal tissues and structures supporting teeth (periodontal ligament, alveolar bone), which is called periodontitis. When the abscess hasn’t spread to periodontal tissues or is just restricted to the gum tissue surface and interdental gum area, it is called a gingival abscess (gum abscess). The cause of a periodontal abscess is poor oral hygiene and accumulation of dental plaque. This condition can cause loose teeth and eventually leads to tooth loss.
Signs and symptoms of dental abscess
The dental abscess’ symptoms can vary depending on tooth abscess and its stage. Generally, you will feel:
- A painful toothache which is sourced from the offending tooth and is continuous and throbbing. The pain can be felt in the area near the affected tooth and the surrounding gums.
- Fever
- Swollen face and cheeks
- Teeth sensitivity when exposed to hot or cold foods/drinks, air, and even sweets
- Swelling in the lymph nodes which is visible in your neck and in the jaw
- Swollen and red gums that can easily bleed
- Loose tooth or teeth. Your teeth can feel tender to pressure and are loose
- Pain in the ear, jaw, and neck
- Swallowing and breathing difficulties
- Bad breath and appearance of foul taste and smell in your mouth
See your dentist or nearby care provider immediately in case of any of these signs and symptoms to treat your dental abscess. Don’t delay in seeking treatments since the infection from your tooth abscess may progress to other parts of the body. Difficulty in breathing or swallowing are some emergency signs that you should be treated promptly by your dentist or the doctor.
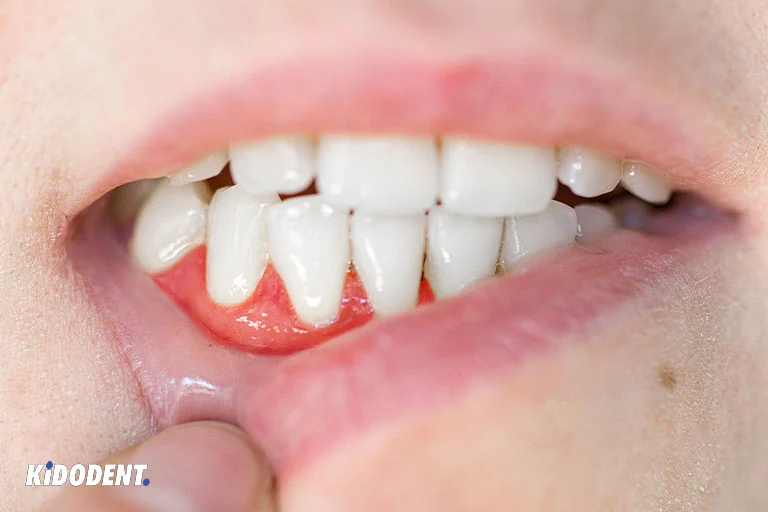
What causes dental abscess?
Poor oral health is the primary cause of the dental abscess. When you are not brushing or flossing regularly, plaque builds up on your teeth and causes tooth decay and cavities. The bacteria in the plaque will enter the pulp through the cavities on your teeth and result in pulp infection. Ultimately, the infection spreads to the root of the tooth and causes abscess formation.
For periodontal abscess, the accumulation of plaque on teeth will lead to bacterial activity in the periodontium and the formation of a periodontal pocket or gap. The infections as a result cause a periodontal abscess.
Other major causes of a dental abscess include:
- Diets high in sugar and acidic foods and drinks.
High-sugary diet is associated with tooth decay. When you frequently eat sweets and candy and drink sugary/acidic beverages, you will contribute to plaque accumulation and speed up the decay process of your teeth. This in turn weakens enamel and reinforces dental cavities sooner.
- Dental injures.
Tooth injuries like cracks and chipping or deeper dental damage will leave the underlying dentin and dental pulp susceptible and open for infections. Therefore, don’t let your damaged tooth go untreated and seek dental restoration with composite dental bonding, dental crown, or inlay and onlay teeth restorations depending on what dentists recommend.
- Dry mouth or saliva disorders.
One of the main risk factors for tooth decay is dry mouth. This condition is caused by changes in saliva production in your mouth, which is a natural moisturizer and teeth cleanser. Dry mouth can be due to the medication you take or because of aging issues.
- Underlying conditions.
People with immunocompromised conditions and individuals with certain conditions like cancer and diabetes are at higher risk of tooth abscess.
How is dental abscess treated?
The goal of dental abscess treatment is to get rid of infection immediately and then restore gum and dental health. Therefore, your dentist will treat a tooth abscess by draining the pus first. Your dentist or endodontist work out the treatment options through:
- Surgical incision/draining the abscess.
The dentist and endodontist will make a small incision (cuts) on the abscess to drain the pus. This allows for swelling to diminish and the abscessed mass area to rupture. They will then wash and disinfect the area with salt water.
- Antibiotics.
Your dentist can prescribe antibiotics to eliminate bacteria and to get rid of further development of infections. Antibiotics are especially recommended when there are risks of the systematic rise of bacterial growth.
- Root canal treatment.
When the infection spreads to a dental pulp in the tooth roots, the root canals inside the tooth should be cleaned off of the bacteria, sealed, and filled with special material to save the tooth. This procedure, which is called root canal treatment, can be done by either a general dentist if the process is not difficult or an endodontist who has advanced expertise in endodontic therapy. Then your upper part of the tooth is restored with a dental crown if the tooth is severely worn down or other restorations like composite dental restorations if it is repairable with these methods.
- Extraction of the infected tooth.
In situations when an infected tooth can’t be saved and should be pulled out, your endodontist or dentist will extract the tooth. After that, they will drain the abscess to stop the infection. Your lost tooth, later on, will be replaced with a dental implant.
Dental abscess pain relief
Visiting a dentist for treatments is the best way to get rid of a tooth abscess infection. If pain is unbearable before you go to the dental clinic or emergency room, you can take over-the-counter painkillers to prevent more discomfort. Remember that pain medications can also be prescribed by your dentist both before or after the abscessed tooth is treated.
Some home remedies like salt water rinse can help decrease the pain. Or, putting an ice pack on the aching tooth, which is also recommended after extracting the tooth, is a helpful home pain reliever.
All these are for the purpose of relieving the pain temporarily and not a treatment at all.
Risk factors and complications of a dental abscess
A tooth abscess doesn’t resolve on its own and requires treatment as soon as possible. The infection causes serious health risks and severe outcomes when there is a delay in treatments. The risks of infection spreading to other parts of the head and neck area gets high when it is left untreated. Some of the complications of a tooth abscess include:
- Sinus infection.
The infection from the abscessed tooth can spread to other oral soft tissues of the mouth like the sinus.
- Tooth loss.
The dental abscess will sometimes cause the offending tooth to be affected so severely that it should be removed. Whether it is a periodontal abscess or a periapical abscess, the tooth should be extracted and replaced with an implant.
- Spread of infection to the jawbone.
The untreated tooth abscess can spread to the jawbone and other bone structures near the abscess.
- Sepsis.
If the infection enters the bloodstream, it causes sepsis and is a serious, life-threatening condition.
How to prevent an abscessed tooth?
The best prevention tip for tooth abscess is good oral hygiene. You can prevent the risks of developing any oral and dental problems and dental abscess included if you follow the below tips:
- Brush your teeth with fluoride toothpaste twice a day. Use an electric toothbrush for an enhanced brushing experience.
- Floss regularly to get rid of food impactions between your teeth. You may use regular dental floss or water flosser to clean the interdental spaces thoroughly.
- Change your toothbrush or the electric brush head every three months.
- Get on with healthier eating and lifestyle like cutting down on high-sugar foods and drinks and quitting smoking
- Swish your mouth with an antibacterial or a fluoride mouthwash from time to time to get bacteria-killing benefits and strengthen your teeth
- Have regular dental check-ups to detect signs of tooth decay in the first place and prevent abscess formation. Your dentist can also perform a professional teeth cleaning and remove plaque buildups that are hardened on your teeth (tartar) which otherwise cannot be removed at home.